Canine superficial pyoderma poses diagnostic and therapeutic challenges due to a varied clinical presentation, and the frequent presence of underlying diseases that impair immunity or compromise skin barrier function. Failure to recognise these underlying diseases will result in relapses even if the superficial pyoderma responds to initial treatment. Repeated prescriptions will then increase the risk of selecting for multidrug resistant bacteria, one of the major threats to human and animal health currently.
The causative bacterium in most cases is Staphylococcus pseudintermedius (formerly S. intermedius). Other staphylococcal species, such as S. schleiferi and S. aureus, or Gram-negative rods are less frequently isolated.
Traditionally, canine pyoderma has been classified according to the depth of infection as surface, superficial or deep
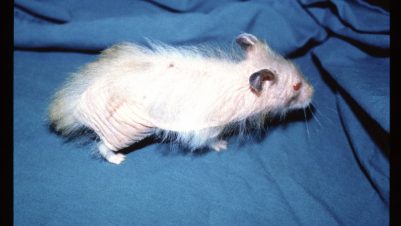
Traditionally, canine pyoderma has been classified according to the depth of infection as surface, superficial or deep. The classical lesions in superficial cases are pustules, which may involve hair follicles. Pustules tend to be transient and other lesions such as epidermal collarettes (Figures 1 and 2), papules (Figure 2), crusts (Figures 1 and 3) and (in short-haired dogs in particular) moth-eaten alopecia are more frequently seen.
Clinical signs are often sufficient to classify the depth of infection, once the lesions are recognised as pyoderma. Superficial infections extend to the level of the intact hair follicle and can be between follicles or involving follicles.

Potential problems
Most problems associated with recurrent canine superficial pyoderma arise from three main areas: difficulties in diagnosis of the pyoderma itself and underlying causes; the presence of antimicrobial resistance; and owner compliance.
Diagnostic problems
- Lesions not initially being recognised as bacterial
- Failure to recognise or difficulties investigating underlying causes
Treatment problems
- Antibacterial therapy not effective against the causative bacterium
- An effective agent used but at an incorrect dose or for insufficient time
- Presence of a multi-resistant organism
- Failure to treat underlying disease – a major cause of recurring cases
Underlying causes of canine recurrent superficial pyoderma may be (after Hnilica and Patterson, 2017):
- Demodicosis
- Scabies
- Other ectoparasites
- Hypersensitivity – fleabite, atopy, food
- Endocrinopathy – hypothyroidism, hyperadrenocorticism, sex hormone imbalances
- Anti-inflammatory or immunosuppressive therapy
- Autoimmune and immune-mediated disorders
- Trauma or bite wound
- Any chronic skin disease
Compliance problems
Recurrent canine superficial pyoderma inevitably involves quite complex concepts and requires a dedicated owner.


Considerable communication is involved and adequate time will need to be found. Common problems include the inability to treat the dog topically, not finishing the antibacterial course and the costs involved in both treatment and investigation of underlying causes.
Making a diagnosis
In recurrent superficial pyoderma cases, it is important to differentiate between true recurrence and resistance/ treatment failures. A detailed history is essential. True recurrence is in those cases where the problem is correctly treated and resolved but recurs at a variable time due to an ongoing underlying cause or immune system deficiency. Additional detailed history taking is essential to enable diagnostic tests to be focused on potential underlying factors.
The main differential diagnoses are:
- Demodicosis
- Dermatophytosis
- Scabies
- Pemphigus foliaceus
- Other underlying diseases listed above
Two diagnostic tests are available to enable an accurate diagnosis. Firstly, cytological examination will confirm the presence (or absence) of bacteria. This is advised in every case. It is easy, quick and extremely cost effective. Secondly, culture of pathogenic bacteria followed by antimicrobial sensitivity testing will identify the target organism and
With the increasing emergence of multi-drug resistant bacteria, culture and antimicrobial sensitivity testing is of extreme importance
aid selection of appropriate drugs if systemic drugs are indicated. Note that growth of bacteria from a skin sample in the absence of cytological examinations may not confirm a diagnosis of pyoderma, as it is possible for microflora organisms to be cultured even from healthy skin.
Tape stripping
Clear adhesive tape is applied to lesion sites, stained with Diff-Quik and examined using the X100 oil immersion objective. In mixed infections, rods and cocci may be seen. Tape stripping may also isolate Demodex mites.
Direct impression
Direct impression with a glass slide is very useful when pustules are present. These can be punctured using a sterile needle and the glass slide applied to the pus, before air drying and staining. Usually, large numbers of degenerate neutrophils with intracellular and extracellular cocci are present. Sampling of epidermal collarettes can be obtained by impression smears of inflamed skin under peeled-back scale.
Bacterial culture
With the increasing emergence of multi-drug resistant bacteria, culture and antimicrobial sensitivity testing is of extreme importance. It is never contraindicated. If multi-drug resistance becomes more common it is likely that culture and sensitivity testing will be considered mandatory and the use of empirical antimicrobial treatment will cease entirely.
Therapy options
Until recently, virtually all cases of superficial pyoderma could be treated with oral antibiotics. In many instances, these drugs were used empirically since the main pathogen, S. pseudintermedius, was sensitive to many antibiotics and resistance was rare. The recent rise of multi-drug resistance has prompted the strongly advised use of topical therapy as an initial treatment for superficial pyoderma.
Suitable topical products include chlorhexidine, either alone or in combination with miconazole, benzoyl peroxide, ethyl lactate shampoos and products containing sodium hypochlorite and hypochlorous acid.
Efficacy comparable to systemic antibiotics has been shown for chlorhexidine products and to date, clinically relevant resistance to topical therapy has not been reported. In addition, some multi-drug resistant skin infections have been shown to respond to topical therapy alone – particularly with shampoos containing chlorhexidine.
Systemic antibiotics may be required if topical therapy fails or is not practical. Traditionally, those antibacterial drugs effective against S. pseudintermedius have included potentiated sulphonamides, clindamycin, first generation cephalosporins (such as cephalexin) and co-amoxyclav. If empirical treatment has been used with any of the above drugs, it is suggested that only one course should be prescribed and in the event of failure or recurrence, culture and sensitivity testing should follow.
Guidelines for the judicious use of antibiotics in the treatment of superficial pyoderma have been published (Hillier et al., 2014).
It is important that the right antibacterial agent is chosen. Equally important is the need for an adequate duration of treatment. Most cases show improvement within two weeks and it is suggested that as a minimum, a course should be for three weeks.
More severe cases may require longer and it is recommended by most texts to continue for a week after resolution of all signs. Further study is required to justify this statement but in the absence of evidence to the contrary, it is suggested that conventional protocols in treatment are followed.
Summary
There are considerable potential problems in the diagnosis and management of recurrent canine superficial pyoderma. These include: recognition of the various lesions and evaluation of underlying causes, identification of the pathogen, selection of appropriate antimicrobial agents of adequate dose duration, and cost and compliance problems.
It is important to eliminate bacterial infection before considering the use of glucocorticoids. Pyodermas are infections and therefore require antibacterial therapy. This alone will, if correctly instigated, clear lesions in most cases, allowing investigation of underlying causes. Glucocorticoids will mask any underlying pruritic cause and will suppress the antibacterial effect of the immune system.
The increasing issue of antimicrobial resistance has highlighted the need for a responsible approach to how we treat canine recurrent superficial pyoderma. More cytology and more bacterial culture allied to good antimicrobial stewardship will help solve many of the problems.
Topical antimicrobial therapy, effective management of underlying causes and alternatives to systemic antimicrobial therapy, such as autogenous staphylococcal bacterin therapy, should be considered. The most serious cases, especially those involving multidrug resistance, will benefit from referral to a veterinary dermatology specialist.






-1628179421-401x226.jpg)



