You need to register to access this content. Registration is free and can be done below. Alternatively, you can log in or join our membership for unlimited CPD content.
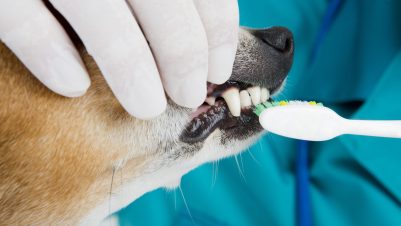
Oral examinations in the consult room
An oral examination should be performed at all consultations to minimise the risk of painful dental disease later on