About 18 months ago, I “outed” myself as having an interest in pseudopregnancy in dogs. This has resulted in a steady mudslide of emails from veterinary practices, behaviourists and owners needing help, and me realising much of the readily available information is sparse, inadequate and behaviourally indifferent. This article is an attempt to elucidate the critical points that are lacking, thus supporting caregivers to ameliorate or avoid negative behavioural tendencies linked with pseudopregnancy.
Myth one: all pseudopregnant dogs produce milk
This is the biggest myth of all! Clinical signs of pseudopregnancy can be physical and/or behavioural. While lactation is one of the most common physical signs, its absence does not rule out a diagnosis of pseudopregnancy. Some cases of pseudopregnancy only have behavioural signs (Root et al., 2018).

The most common physical signs (Root et al., 2018) are:
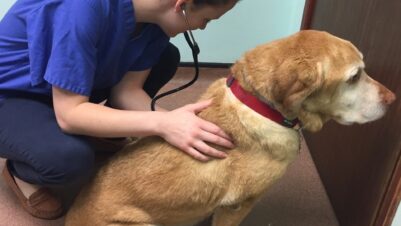
- Mammary enlargement (Figure 1)
- Lactation
These are followed, some way back, by:
- Weight gain
- Abdominal distension
- Abdominal contractions
- Vomiting
- Diarrhoea
- Polyuria
- Polydipsia
The most common behavioural signs (Root et al., 2018) are:
- Collecting and mothering of objects (Figure 2)
- Nesting behaviour
These are followed by:
- Changes in activity levels (increased or decreased)
- Inappetence
- Aggression
Some of the less commonly recognised signs are:
- Anxiety
- Increased reactivity
- Over affection
- Licking
- Destruction
- Polyphagia

Recognising that just one or more of the physical or behavioural signs above could indicate a pseudopregnancy is important, as diagnosis of pseudopregnancy is based purely on history and clinical signs. Hormonal assays are non-diagnostic for pseudopregnancy (Gobello, 2021; Root et al., 2018), as all bitches experience the same hormonal changes regardless of whether they are displaying clinical signs (“overt pseudopregnancy”) or not (“covert pseudopregnancy”). The hypotheses behind overt versus covert pseudopregnancies include differing individual sensitivity to prolactin and prolactin having different molecular variants with different biopotencies (Gobello, 2021; Root et al., 2018). The exact frequency of occurrence of overt pseudopregnancy is unknown, and estimates vary, but it is more prevalent in some breeds (Gobello, 2021; Root et al., 2018). These include Dalmatians, Boxers, Pointers, Dachshunds, Bassett Hounds and Afghan Hounds.
Recognising that just one or more of the physical or behavioural signs […] could indicate a pseudopregnancy is important, as diagnosis of pseudopregnancy is based purely on history and clinical signs
So, one or more of the physical or behavioural signs listed, occurring within a few weeks of a season (typically 6 to 12 weeks), should arouse suspicions of pseudopregnancy. Pyometra and pregnancy should also be on the differential diagnosis list and can be excluded by diagnostic tests. Pregnancy is important to rule out as cabergoline, the treatment of choice for pseudopregnancy in bitches, can cause abortion. Further, the treatment for pyometra includes spaying and this is contraindicated in pseudopregnant bitches (Gobello, 2021; Harvey et al., 1999; Root et al., 2018).
Myth two: there is no need to use medication as pseudopregnancies are normal and resolve on their own
If only I had a pound for every time I have heard this! It is true that pseudopregnancies are normal and resolve spontaneously, but there are occasions when treatment is advisable.
Following a diagnosis of pseudopregnancy, the options are to:
- Do nothing
- Treat conservatively
- Treat medically
Doing nothing is not without risk. In lactating bitches, there is the risk of mastitis and/or loss of condition. The jury is still out on whether repeated pseudopregnancies predispose bitches to mammary tumours (Gobello, 2021; Romagnoli, 2009), but it remains concerning. If aggression is being displayed, bites to humans, dogs or other animals are a major concern. With any of the behavioural signs, the risk of behaviours being learned, and remaining to some degree post-pseudopregnancy, is ever-present. Further, it is important to consider that while many straightforward pseudopregnancies last two to four weeks, they can persist until the next oestrus cycle (Gobello, 2021).
Conservative treatment includes removing the mothered objects, preventing mammary stimulation (with a post-surgical recovery suit or an inflatable collar), increasing exercise and short-term dietary restrictions (Hermo et al., 2009). This may help alleviate clinical signs sooner, thus reducing some of the above risks, but it may not. Medically, as mentioned, cabergoline is the drug commonly used (Gobello, 2021; Root et al., 2018), and licensed in the UK, for treating pseudopregnancy in bitches. There are other less effective treatments for pseudopregnancy, both licensed and unlicensed, but they are beyond the scope of this article.
Treating medically
Cabergoline is a dopamine agonist and inhibits the release of prolactin (the hormone responsible for the signs of pseudopregnancy) from the pituitary gland. It is licensed at a dose of 5µg/kg once a day (preferably with food) for four to six days. Sometimes, treated pseudopregnancies recur within the same cycle and will need repeat course(s) of treatment. Due to the long duration of binding to pituitary receptors, cabergoline continues to be effective for a few days after the last dose. It reduces mammary enlargement, lactation and behavioural signs. (Recently I have encountered information suggesting it does not treat the behavioural signs – a “mini myth” – it does.)
Please note that in those dogs with aggression-related behavioural signs, 14 days of cabergoline may be required (Ramsey, 2017). Currently, I recommend 14 days for any dog with aggression or anxiety resulting from pseudopregnancy.
There are some side effects and contraindications to consider with cabergoline (which can easily be found in the SPCs/datasheets for the licensed products), but these are far fewer than other licensed and most unlicensed products. Cabergoline has a longer duration of action and it is more effective (Gobello, 2021; Root et al., 2018). While safe and effective, it is expensive. This cost must be weighed against the benefits of an earlier resolution, and the avoidance of lengthy and costly behaviour therapy in dogs where undesired behaviours have become learned.
These are the situations in which I am more inclined to recommend treatment with cabergoline:
- Excessive milk production
- Painful mammary glands
- Loss of condition
- Where “do nothing” or conservative treatment has been adopted, yet signs persist
- Aggressive behaviour – especially in households with vulnerable people, in multi-dog households and/or in mixed-species households
- Behaviour (not just aggression) is causing problems for the client
- Behaviour (not just aggression) is causing concern for the welfare of the dog for the client, vet or other paraprofessionals
- Pre-existing behavioural issues on which we do not want to add a layer of learning
- Previous history of pseudopregnancies resulting in problematic clinical signs
The decision to use cabergoline should be based on the degree to which the dog’s welfare is, or is likely to be, negatively affected by pseudopregnancy; the degree of concern it is causing the client, vet or other paraprofessionals; and any public or animal safety implications
In summary, the decision to use cabergoline should be based on the degree to which the dog’s welfare is, or is likely to be, negatively affected by pseudopregnancy; the degree of concern it is causing the client, vet or other paraprofessionals; and any public or animal safety implications. Those thoughts should then be evaluated alongside possible side effects, contraindications and the cost of treatment.
Myth three: a spayed bitch cannot have a pseudopregnancy

I hate to break it to you, but they can and it is unintentionally iatrogenic. It results from spaying a dog in metoestrus/dioestrus (Gobello, 2021; Harvey et al., 1997, 1999; Root et al., 2018) instead of during anoestrus, which is the optimal time to do it. The even worse news is that these pseudopregnancies may not resolve on their own – they may become what is known as a persistent pseudopregnancy (Harvey et al., 1999), also known as chronic pseudopregnancy, chronic false pregnancy or chronic pseudocyesis. It is possible to accidentally trap a dog in a permanent state of pseudopregnancy.
In my experience, they present in one of two ways:
- Within days of spaying, a bitch goes into an overt pseudopregnancy (Harvey et al., 1999) with physical and/or behavioural signs (Figure 3)
- Within a few months of spaying, a bitch develops aggression or anxiety, with or without any of the other typical behavioural or physical signs of pseudopregnancy
I have come across dogs in the second category presenting with either dog–human aggression and/or anxiety, dog–dog aggression and/or anxiety, sound sensitivity and even separation-related behaviours. That’s quite the behavioural “pick and mix”!
when a bitch is spayed in metoestrus/dioestrus the resultant decrease in progesterone is also followed by an increase in prolactin
The precise physiopathology has yet to be elucidated but has been experimentally induced by performing an ovariectomy in metoestrus/dioestrus (Gobello et al., 2001). In the normal oestrus cycle, progesterone increases after ovulation and then decreases. This is followed by an increase in prolactin. When prolactin later decreases to basal levels the dog is in anoestrus. The precise mechanism by which the decrease in progesterone is followed by, or triggers, the increase in prolactin is not known. However, when a bitch is spayed in metoestrus/dioestrus the resultant decrease in progesterone is also followed by an increase in prolactin (Harvey et al., 1999; Root et al., 2018) and pseudopregnancy results. The precise mechanism for the normal tail-off in prolactin is similarly unknown but, whatever it is, when we spay a bitch, we appear to have interfered with that “off switch” as now the pseudopregnancy is persistent. Luckily, it is treatable, and largely avoidable, and will be the focus of a later article.
Summary
In conclusion, pseudopregnancy comes with as many myths as it has names (such as pseudocyesis, nervous lactation, false lactation, false pregnancy and phantom pregnancy). This article should have elucidated the main three and, hopefully, provided evidence to counter them.