Canine scabies (sarcoptic mange) is one of the oldest known skin diseases. It is caused by the superficial burrowing mite Sarcoptes scabiei var canis (Figure 1). Affected animals rapidly develop hypersensitivity to the mite, resulting in severe pruritus.
Clinical features
Scabies is highly contagious and there may be a history of contact with other dogs, also exhibiting pruritus, in kennels, grooming facilities, parks or in the household. In the UK urban foxes are a source of infestation. The condition is progressive without treatment and will become generalised.
Lesions include papules, alopecia, erythema, crusts and excoriations. In the early stages, lesions may be subtle and consist of mild pruritus, scaling and fine crusting, especially on the edges of the pinnae. They then extend to involve the facial area (Figure 2). As the disease progresses, there is involvement of the elbows, hocks, brisket, ventral abdomen and eventually most parts of the body.


Affected dogs may develop systemic signs of disease such as anorexia with weight loss, and a peripheral lymphadenopathy is common. Severely affected dogs will incessantly scratch and bite, causing excoriation (Figure 3). Severe neglected cases can result in death and scabies is also a common cause of death in urban foxes.
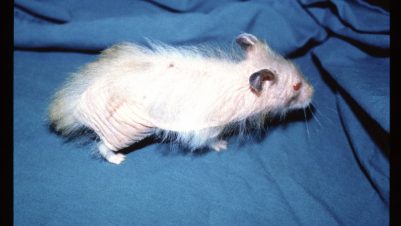
A rare form of the disease is one involving severe generalised crusting, analogous to a human variant called Norwegian scabies. In these cases, there are usually multiple mites and an underlying immune suppression should be suspected.
In a multi-dog household, it is possible that some dogs will harbour mites but not show signs. In time, without veterinary intervention, hypersensitivity develops and these dogs will also become pruritic.
Contagion to humans is common. Lesions occur in contact sites with the dog, arms and abdomen, for example, and are extremely pruritic. These lesions generally spontaneously disappear with appropriate treatment of the dog, although communication with the family physician is advisable.
Differential diagnosis
- Allergic skin diseases (atopy, food, flea)
◽ In the early stages, scabies can mimic atopic dermatitis in particular and respond to anti-inflammatory doses of glucocorticoids. This response is lost as the disease becomes more generalised and there have been cases where even immunosuppressive doses of glucocorticoids failed to control pruritus
- Malassezia dermatitis
- Superficial pyoderma
◽ If combined with Malassezia, the resulting pruritus can be as severe as that of scabies
- Demodicosis
- Dermatophytosis
- Pemphigus foliaceus if severe crusting is present

Diagnosis
A history of severe pruritus, increasing in severity with time, and increasingly poorly responsive to glucocorticoids is suggestive. If acaricidal treatments have been used, it is important to check compliance. Pups bred in poor husbandry conditions are susceptible.
A physical examination should be undertaken with attention to typical lesion sites. Rubbing the ear margin between the thumb and forefinger causes the dog to scratch. This pinnal-pedal reflex is highly suggestive of scabies, although not 100 percent positive. It should prompt treatment even if other tests are negative.
Tape strips should be done to rule out Malassezia and superficial pyoderma. Also take superficial and deep skin scrapings. Multiple samples (up to 10) are advised, as Sarcoptes is very difficult to find except in the Norwegian type mentioned above. Excoriation sites should be avoided. Scrapings can be taken from the edge of lesions. A single mite or egg is diagnostic.
ELISA assay is a useful test in chronic cases. The test detects IgG antibodies against Sarcoptes antigens. It is highly sensitive and specific. False negatives may be obtained in early cases, as there is a time lag of three to five weeks after infestation for seroconversion to take place. False positives may occur due to persistence of antibodies for several months after successful treatment.
Dermatohistopathology is also useful. Non-specific findings include epidermal hyperplasia, superficial perivascular dermatitis with lymphocytes, mast cells and eosinophils (Hnilica and Patterson, 2017). Mite segments are very occasionally found within the stratum corneum and upper epidermis (Figure 4).
In the presence of suggestive clinical signs, and when sampling has failed to find mites, a therapeutic trial is recommended. A product with a licence for Sarcoptes should be selected, and is best administered by a veterinary surgeon or nurse to eliminate compliance problems.
Systemic treatments are suggested for a therapeutic trial for accurate dosing and better compliance (Hnilica and Patterson, 2017). Three monthly checkups are suggested, as most cases will resolve in that time.

Treatment
Canine scabies is not always an easy disease to diagnose but treatment is straightforward in most cases. There is no lack of products with a licence for the treatment of canine scabies and any of them will be highly effective if used according to the manufacturer’s instructions.
Examples of suitable products include sprays (fipronil), washes (lime sulphur dip), spot-on products (selamectin, imidacloprid/moxidectin) and chewable tablets (sarolaner). These examples are not exhaustive and the choice of product will depend on an individual clinician’s preference.
All dogs in the household should be treated, bedding should be destroyed and the environment treated with parasiticidal sprays, using products suitable for flea control.
There is usually a response within two weeks with maximum effect in six to eight weeks. Glucocorticoids may be used to help control pruritus in the first week or so, but only in confirmed cases and not in conjunction with therapeutic trials.
Formulating a year-round parasite control programme that includes measures against fleas, ticks, other mites and endoparasites provides effective protection against canine scabies.
Prognosis
The main limiting factor with scabies treatment is a failure of compliance. Measures taken to avoid this include monthly checkups (with reminders), and nurses or veterinary surgeons administering the treatment. In these cases, the prognosis is very good.







-1628179421-401x226.jpg)



