Canine demodicosis is a common cutaneous disease caused by two species – Demodex canis and Demodex injai. There is a third short-bodied species previously described but currently considered to be a variant of D. canis, and not differing in its clinical presentation. D. canis is the focus of this article.
.jpg)
Demodicosis may be localised, generalised (juvenile onset or adult onset) or demodectic pododermatitis. Some cases of pododermatitis may have originated as generalised cases but not resolved, while others present just with pododermatisis but are still considered under the generalised heading.
Generalised demodicosis due to D. canis is one of the oldest dermatoses to be described in veterinary literature. In the Middle Ages, it was known as “redde mange” due to the erythematous lesions of some cases (Figures 1 and 2). Juvenile onset demodicosis is the most common type of generalised case and is described here.
Until recently, juvenile onset demodicosis was considered a difficult condition to cure and earlier texts warned that euthanasia needed consideration in the most advanced cases. Recent advances in treatment have altered this guarded prognosis into a favourable outcome for the majority of affected dogs.
.jpg)
It is known that a genetic predisposition to develop generalised juvenile demodicosis exists. The primary defect leading to the disease is unknown, however. With advanced mite proliferation, dogs develop T-cell exhaustion favouring increasing mite proliferation and secondary pyoderma. Treatment with effective acaricidal products reverses T-cell exhaustion and leads to a clinical cure. It is unclear why some dogs develop generalised demodicosis at a young age and why these dogs after treatment usually remain cured. If there were an underlying primary genetic cause, it would be logical to expect relapse to be common, but that is not the case.
.jpg)
It has been suggested that dogs with demodicosis have an inherited Demodex specific T-cell deficit of varying severity (Miller et al., 2013). This would explain the higher incidence in some breeds and why not all pups in a litter suffer from demodicosis. Indiscriminate breeding of dogs such as Staffordshire Bull Terriers by back street breeders has led to a marked increased incidence of the disease in
recent years in the UK.
There are four stages to the life cycle: eggs (lemon pip shaped), six-legged larvae, eight-legged nymphs and eight-legged adults. The mites are transferred from the mother to the pups in the first two to three days of life, which explains why lesions tend initially to involve facial and pedal regions. After initial transfer of mites has occurred, the disease is non-contagious.
Clinical features
Canine generalised demodicosis is much more commin in pedigree dogs although, particularly with indiscriminate breeding, many breeds may be affected. A recent study in the United States identified the American Staffordshire Terrier, Chinese Shar-Pei and Staffordshire Bull Terrier as predisposed breeds (Plant et al., 2011). With indiscriminate breeding of dogs deemed to be popular and not normally thought to be predisposed, eg the Chihuahua, cases of demodicosis may be seen. In the author’s series, many dogs have been Staffordshire Bull Terriers or their crosses.
.jpg)
.jpg) FIGURE (5) The dog in Figure 4 showed significant improvement following treatment over two months
FIGURE (5) The dog in Figure 4 showed significant improvement following treatment over two monthsLesions
The distinction between localised and generalised cases differs slightly between veterinary dermatologists but a consensus is five to six patches, or one area of the body widely affected, and/or more than two feet suggested as defining the generalised condition. Most cases seen by the author have involved large parts of the body and have developed rapidly. The disease usually begins before 18 months of age with the majority in the first year of life:
- Numerous lesions appear on the head, legs and trunk and eventually occur everywhere
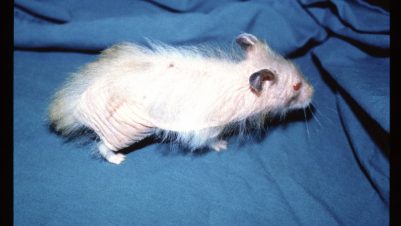
- Patches of alopecia become more genearlised (Figure 4)
- Scaling and erythema (in many early cases, the erythema may be quite pronounced, as mentioned above, and is an important diagnostic clue)
- Later, hyperpigmentation is seen with grey or blue-grey colour (this is also an important diagnostic clue; Figures 4 and 7)
- Staphylococcus pseudintermedius is the most frequent pathogen to be isolated but in severe cases, other opportunist bacteria such as Pseudomonas or Proteus may be present
- Lesions of the skin of the feet (demodectic pododermatitis) are invariably features of generalised demodicosis, but some cases present with foot lesions alone (Figure 7). Often these cases are chronic with hyperpigmentation and skin thickening
Diagnosis
Undertake a full history and physical examination. The history is particularly important, as the disease may be missed initially and continue into adulthood. A distinction needs to be made whether the dog has juvenile onset or adult onset
disease. Cases that began after two years of age, and in most instances older than this, are adult onset and more difficult to cure due to concomitant immunosuppressing disease. Juvenile onset disease has a much better prognosis.
As the consequences of not diagnosing the disease are considerable in terms of welfare and cost, it is suggested that time is allocated for adequate sampling to maximise the ability to make a diagnosis. It is more difficult to do this
within the constraints of a normal consultation and either sufficient time can be allocated, or the dog admitted for sampling and scanning of slides. Trained veterinary dermatology nurses can be invaluable for these procedures.
.jpg)
Sampling techniques
Rather than rely on just one sampling technique, it is suggested that several procedures performed sequentially on an affected dog may help to maximise success in finding the parasite. These can be done in the following order:
- Hair plucks: This simple technique may show mites in hair follicles. It is very useful in areas where more invasive techniques could cause damage to the dog or sampler, for example in the feed and periocular regions.
- Adhesive tape preparations: Tape strips (preferably ultra-transparent) are pressed against lesions and the tape is transferred to a microscope slide. This is another useful non-invasive technique in difficult-to-sample areas but also where secondary infection has produced an exudate.
- Impression smears with a glass slide: These are often successful where there are exudative lesions (Figure 6).
- Skin scrapings: The skin is squeezed first and scraping performed in the direction of hair follicles using a blunt scalpel blade. The area to be scraped may need clipping, after which liquid paraffin is applied to the skin surface. This enables material to adhere to the blade. Deep scrapings, causing capillary ooze, are necessary.
The intial three tests can be performed in a matter of minutes, with the scrapings taking a little longer. The bulk of time necessary to rule the diagnosis in or out is taken up with careful scanning of the microscope slides. This is done under low power, facilitating efficient slide scanning. Generalised cases often yield high numbers of mites; however, a failure to diagnose the condition may be due to inadequate time to perform the procedures outlined above (or not doing them at all) and/or not spending sufficient time at the microscope. With suggestive clinical signs, finding a few mites on a slide should be considered diagnostic, as it is very rare to find mites in healthy dogs.
In spite of the above, there will be some cases that defy attempts to isolate the mite. In these cases, a biopsy is necessary, particularly if there is a strong suspicion based on the history and physical examination. Biopsy is a very useful procedure in difficult-to-sample areas and in chronic cases with lichenification. General anaesthesia or deep sedation is required and the histopathologist should be made aware that demodicosis is suspected. It is not uncommon, however, for the histopathologist to make the diagnosis where the clinician has overlooked that possibility. This has happened to the author who was very grateful at the time!
Treatment
Since medieval times, there have been numerous treatments for generalised demodicosis. Recently, there has been a dramatic improvement in the prognosis with new products, and only those licensed in the UK for the treatment of demodicosis are considered here.
Acaricidal products
Isoxazolines are a new class of ectoparasiticide. They are potent inhibitors of arthropod nervous systems, working by antagonizing GABA and glutamate receptors.
Fluralaner (Bravecto, MSD) was the first of these new compounds demonstrating efficacy against demodicosis. A small study (Fourie et al., 2015) reported reduction in mite numbers of 100 percent at days 56 and 84 following a single
oral administration at 25mg/kg. Since this initial publication, there have been many case studies showing similar results. Bravecto is administered orally at a dose of 25mg/kg every 8 to 12 weeks.
.jpg)
.png)
The isoxazolines are now considered first-choice treatments for generalised demodicosis and will perhaps remain so for the foreseeable future. Other equally effective isoxazoline (oral) products include: Afoxolaner (NexGard; 2.7 to 6.9mg/kg every two weeks); Sarolaner (Simparica; 2 to 4mg/kg every four weeks); Lotilaner (Credelio; 20mg/kg every four weeks).
Oral administration allows for much better compliance in comparison to other licensed products and to date there have been few side effects of any importance.
For many years, amitraz (Aludex) has been an effective treatment for generalised demodicosis as a weekly wash at a concentration of 500ppm. Side effects included mild sedation, especially with the first few applications, and in a few
cases, bradycardia, ataxia, polydipsia, polyphagia and pruritus. The product needs to be applied in a well-ventilated room and protective clothing is necessary.
Moxidectin 2.5 percent combined with 10 percent imidacloprid (Advocate) can be applied as a spot on at a dose of 2.5 to 5mg/kg weekly. Side effects occasionally include transient lethargy, anorexia and ataxia.
In the past, treatment failure has often been associated with compliance, as a dedicated owner sticking to treatment protocols was crucial. Additionally, many generalised cases are secondarily infected with Staphylococcus pseudintermedius and failure to treat secondary pyoderma effectively is a potent cause of failure. The presence of a secondary pyoderma is easily assessed by cytological examination, either with impression smears or tape strips.
Antibacterial products
Deep exudative pyodermas should be treated with systemic antibacterial agents, based on culture and sensitivity testing, until clinical resolution plus a few weeks. Many less severe cases of pyoderma may respond to topical therapy using antibacterial shampoos, such as those containing chlorhexidine, thus avoiding the use of antibacterial agents in the long term.
A consensus view worldwide is that in order to diminish the incidence of demodicosis, affected dogs or their parents should not be used for breeding.